Improving the quality of healthcare and access to healthcare while controlling costs as populations age and grow, life expectancy increases and public expenditure on healthcare is under pressure are a few of the main challenges for healthcare organizations across the globe.
Virtually all the players in the vast and complex healthcare ecosystem are stepping up their digitization and digital transformation efforts as a result of these and other challenges but they also see the opportunities in digitally transforming healthcare and invest more in digital health.

The ‘organization’ of healthcare is different across the globe and healthcare organizations are moving at different speeds, depending on country, legal framework, political agenda, individual organization, role in the healthcare ecosystem and the precise goals of digital transformation within each individual context: from enhancing patient-centricity in hospitals and improving workforce conditions to new ways of care, for instance remote health monitoring by leveraging cloud computing and the Internet of Things.
The many aspects of digital transformation in connected/digital healthcare
If you look at the vast healthcare ecosystem (with providers and payers as two key sub-ecosystems) and where digital technologies – with a clear purpose in any given context – fit in, you can wonder what digital transformation in healthcare even means?
Is it about leveraging digital technologies in novel ways to improve health? Is it about leveraging digital technologies in order to make healthcare more affordable and cost-effective (which is a universal need)? Is it about finding new revenue sources as healthcare does need to be funded? Is it the digital transformation of an entire industry in nations where healthcare tourism is seen as an importance source of revenue, among others in some countries which were more dependent on oil and are transforming to become service economies?
Is digital transformation also about the digitization of healthcare records (EHR, short for electronic health record, and EMR, short for electronic medical records, as the graphic below shows still a major investment area in the so-called digital health space and a topic we’ve tackled many times before)?
Is it about using Big Data for better healthcare? Is it about enhancing that patient-centricity, for instance by using EHR? About leveraging the Internet of Things in healthcare to enable individuals to improve their health, using those personal healthcare devices? Or rather about the Industrial Internet of Things component where we see remote healthcare (monitoring) as a key IoT use case? Maybe it’s about leveraging technologies such as artificial intelligence, IoT, robotics and new types of sensors to come up with better ways to give patients a better life with new or improved ‘tools’? Or the very funding and organization of healthcare ‘business models’?
Well, digital transformation in healthcare is about all that and more.
Healthcare and digital transformation challenges and considerations
However, digital transformation in healthcare isn’t just about the technological evolutions (digital transformation never is about that first).
It’s about the challenges we need to address in healthcare across the entire ecosystem and all aspects, innovation and building a viable healthcare future, leveraging all those technologies and gigantic sources of predominantly unstructured data and information.
We mention a few (more) healthcare challenges below as they drive digital transformation technology agendas, although in healthcare some technologies are transforming how you will live as well.
Security and patient data challenges
It’s not a secret that there are quite a few of those challenges. Costs, aging populations, changed patient expectations and, let’s certainly not forget: the tough circumstances in which doctors, nurses and healthcare workers overall (very often) need to work.
On top of the broader challenges – and opportunities – facing healthcare and calling for digitization and digitalization or digital transformation there are the “side-effects” which need to be looked at, right from the very start: the challenges regarding security, privacy and compliance in an industry, full with very personal data (clearly covered in the GDPR) that will be leveraged in ways you might not know or expect yet but of which you’ll discover a few below.
However, these additional challenges, such as security and protection of patient data exist beyond the digitalization picture as well. It often even boils down to organizational aspects or the errors of one actor in an overall healthcare ecosystem – and digital transformation involves organizational aspects too.
Take the example of what happened in the UK over the past few years and surfaced early 2017. While the NHS (the national health services in the UK) has an agenda to go paperless, an NHS contractor managed to store correspondence between doctors and hospitals in a warehouse instead of getting it where it belonged. In total approximately half a million confidential NHS correspondence would have been stored instead of sent and, although the government says that there were no risks, it’s not hard to see that, among all that correspondence with diagnosis, medical test results and so forth, cases will pop up with likely patient harm.
Don’t think this is just happening in the UK. It is just one of many examples of how things can go wrong – and do go wrong – in a non-digital context as well – and, when done properly, could be avoided by digitizing information carriers, test results and patient files, with security by design as a must.
The increasing digitization and focus on data in digital transformation and connected healthcare initatives will not be overlooked by ‘the bad guys’ of course. Among others given the importance of data for healthcare, it is expected that attacks will go up.
Healthcare and cybersecurityImproving lives of patients and people
There is of course also the challenge of making healthcare better, from the perspective of patients and other stakeholders.
There are the healthcare workers but, first and foremost, the patients. Healthcare is about them. And here we see amazing evolutions thanks to new technologies.
By way of a specific example take the evolutions in bionic limbs (it just is one of many examples, we could look at all sorts of fields and even specific diseases).
Today, people who have lost (parts of) their arms and legs already dispose of newer brain-controlled bionic limbs that can make their lives easier. Yet, in practice these bionic limbs require a lot of effort from patients and in no way come close to offering the same possibilities as the ‘original’.
Recently we’ve been talking to some firms and members of an innovation project in the field of bionic limbs (which we’ll cover in a separate piece) and the evolutions are simply amazing. If you look at how some recent innovations and coming innovations, which aren’t commercialized yet, will make lives of people who need bionic limbs so much easier (there is a lot of AI, sensors and human reflexes going on), the difference between these bionic limbs with the current generations is just amazing.
The aging population – a digital transformation challenge in healthcare and far beyond
If you have read about digital transformation and overall challenges in healthcare you undoubtedly encountered the aging population.
However, we do tend to underestimate the simple fact that people live longer – and will probably live even longer, among others to…improvements and technological advances in healthcare, and the fact that in many countries growth rates are dropping and, even where this is not the case, the age balance is shifting.
It is expected that by 2050 over 1 in 5 people globally will be years or older and that the number of people aged 60 and over will have doubled in comparison with 2000. In fact, in some countries, there are already more than 25% people aged 60 or older. In Japan, 26.3 percent of the population is even over 65 (not 60 but 65) years old, in Italy that’s 22.4 percent, in Greece 21.4 percent and in Germany 21.2 percent. And 2050 is still a long time away.
An aging population also means that less people are ‘active’ and are able to contribute to healthcare systems funding.
This and many other consequences leads to more healthcare costs and at the same time drives new solutions for the less mobile, while saving costs. It’s not a coincidence that remote healthcare monitoring is and continues to be the major area in Internet of Things spending in healthcare worldwide, although there are more reasons for this than aging populations.
But there is more. With aging populations also comes an increase of chronic diseases, which are typical for older people.
As Richard J. Hodes, M.D, director of the National Institute on Aging puts it: “People are living longer, but that does not necessarily mean that they are living healthier. The increase in our aging population presents many opportunities and also several public health challenges that we need to prepare for”.
You never know what the future will bring but today these chronic, so-called non-communicable diseases already account for three quarters of deaths across the globe. The economic impact? According to the World Economic Forum only five of these diseases will cost the economy 47 trillion (!) USD by 2030.
Attention though: chronic diseases are not just an issue of an aging (and growing) population – and it wouldn’t be fair to look at the ‘elderly’ as if they were just a burden, well on the contrary. There are quite some misconceptions in this regard.
Patient-centricity: meeting – emotional and changed – expectations
Given the key role of the customer, customer-centricity customer experience and user/brand experiences in most digital transformation efforts it probably won’t come as a surprise that the transformational mix of a more digital/mobile lifestyle, changes regarding the way consumers seek healthcare information and increased expectations affect and impact digital transformation in healthcare as well.
We’ve mentioned the so-called spill-over effect several times before and people, in their capacity of patients, do expect more, just as they do in their capacity of consumers and whatnot. Moreover, as healthcare workers are also people last time we checked, there are obviously changes in the behavior and expectations of the workforce too. Needless to say that the rise of ever better and smarter mobile ways of seeking healthcare information, working and, well, doing pretty much anything we can do with mobile devices has played a big role here.
Obviously, as always, context is everything but it would be a mistake to think that people don’t have similar expectations for healthcare as non-healthcare companies. In fact, the assumption that healthcare is different from other industries from this ‘expectation’ perspective is one of several myths which was debunked in an article by McKinsey about healthcare consumerism some time ago. You can find more of those myths in the article.
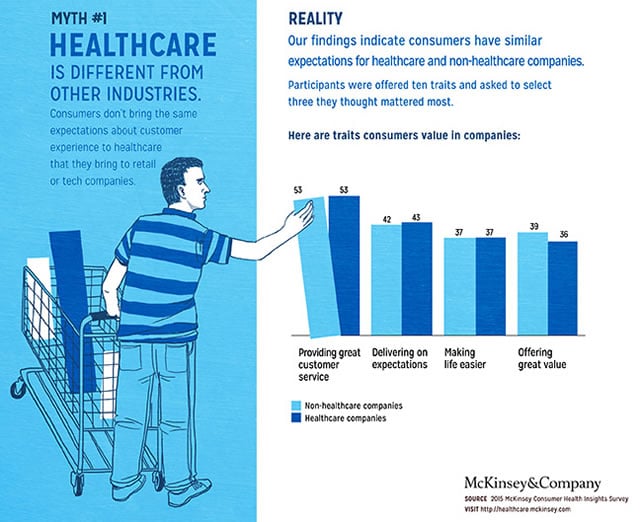
In a sense this shouldn’t surprise us that much though. On top of the mentioned spill-over effect, people have pretty universal demands and needs.
- Most of us hate complexity in dealing with organizations, including healthcare facilities, and want things to run smoothly and be simple. In important decisions or urgent situations, this is even more so.
- We also want attention, in the end a big chunk of what customer-centricity and, in the context of healthcare, patient-centricity is all about: put us first and please pay attention to us. Again, in the context of our health or that of our loved ones, this is even more so.
- Thirdly we need to mention information here. We really want to be informed about our options and seek a sense of security, reassurance and having made the right choices. We want to know what exactly the side-effects of that drug are, we want to know what will happen next, we want to be informed and reassured.
Depending on the exact circumstance of our interactions with healthcare workers or facilities and on our personality these elements can matter more or less.
And technologies, digitization and digitalization or transformation can play important roles here, keeping in mind that as far as health is concerned, the emotional aspect usually becomes much larger.
On the other hand, healthcare workers have tasks to do and are often overloaded. By eliminating complexity from patient-facing processes, offering clear information and automating parts of the routine tasks that healthcare workers need to do, for instance in an acute care setting, resources can be freed up to meet patient expectations.
At least, in theory. If automation becomes merely cost cutting, nothing changes for the patient (more about that below where we take a look at the human aspect).
Which technologies can help here? Too many to list them all. However, it’s clear that digitizing information streams and patient onboarding is already one area where things can be improved. And, a bit more futuristic: robots could take over specific routine tasks from staff in hospitals.
Healthcare patient/consumer ‘engagement’ and patient responsibility
There is a growth of patient engagement (or consumer engagement in healthcare) since several years now. In a nutshell it’s about the motivation and involvement of people to be more engaged and proactive regarding their health and the various aspects surrounding it.
Think about the usage of wearables and personal healthcare devices but also about a more active involvement regarding the choice of healthcare providers and so forth. Despite being a clear evolution and talked about since years for many consumers it’s still rather unclear. Others aren’t so sure about it. Maybe this has to do with the fact that the consumer engagement movement also is about accountability and responsibility.
Like it or not: healthcare systems and healthcare payers will increasingly take your lifestyle and behavior into account.
Prevention, engagement, accountablity and personal responsibility is the rationale, cost savings and different ways of healthcare funding and insurance systems is the goal, with technologies and data being the means.
Isn’t it good that patients are more ‘engaged’, ‘responsible’, ‘motivated’ and ’empowered’ to take better care of their health? Of course it is. Yet, there are risks. Too much focus on health-related behavior and the impact it has, could reduce the attention for underlying cause in an age where healthcare often works on a symptom level and deeper causes are overlooked. Just look at mental healthcare: the focus is on fast results and longer-lasting therapeutic methods are under pressure in many countries. We tackle these concerns more at the end of this overview.
Nevertheless, there is no escaping (unless you pay the price): hand in hand with all sorts of programs to get rid of bad habits and emphasize the need to take better care of our health, data from wearable devices will be used for health insurance and plans. Moreover, new models will continue to emerge whereby the disclosure of personal health data will be encouraged with all sorts of benefits.
You can of course look at this evolution in many ways. It is not a simple nor ‘neutral’ matter. Anyway, according to IDC, 20 percent more people will be engaged in their health by 2020 because of real-time care plan adjustments with cognitive/AI and data from wearable devices. Moreover, the research firm expects that 20 percent of payers will offer personalized benefits with options to dynamically adapt Premiums or change deductible or copay if you disclose personal health data.
Whether these predictions prove to be correct will depend on countries, healthcare provider and payer systems and regional attitudes but know that this is an important evolution. This is digital transformation in healthcare too.
Mobility: from home and remote care to mobile and wireless health
We’ll cover remote health monitoring and the evolutions to move patients from acute healthcare environments to their homes where post-acute monitoring is poised to increase more in depth in a separate article on the Internet of Things in healthcare.
Yet, remote health monitoring is also part of a broader movement towards home and remote care and mobility overall. Rising hospitalization and treatment costs, along with developments in remote monitoring and wireless communications, create a boom in home-based monitoring, diagnosis and treatment.
Moreover, in regions where access to healthcare is less obvious, mobile healthcare offers an alternative as mobile device penetration is growing and healthcare workers are increasingly mobile as we tackled before. In the infographic in the beginning of our overview you could clearly see the evolutions. The global mobile health market is poised to grow the fastest until 2020, followed by the global wireless health market.
Having mobile access to the right patient information, regardless of place and time also meets the tackled changing patient expectations and the needs of an increasingly mobile workforce.
Digital transformation in healthcare – key evolutions
We mentioned several challenges, evolutions, trends and technologies but what does the near and further future hold?
As mentioned, the overarching theme of digital transformation in healthcare and of the increasing deployment of Internet of Things projects, Big Data, AI/cognitive, robotics and obviously EHR/EMR is data and information, as we move towards an information-driven healthcare. It’s also here that we find most innovations of course, always with those challenges in mind.
2017 is poised to be a year in which US healthcare providers AND payers are significantly stepping up their digital transformation deployments as we tackled. While payers are catching up with providers, we mainly see technological investments in the pillars of the third platform and in the use of the Internet of Things.
Healthcare providers and payers - digital transformation 2017The graphic below, based upon the mentioned article and a February 2017 survey by IDC shows the digital transformation healthcare evolutions for 2017 (in the US), which are mainly driven by IT and not the business. It also shows an overview of some evolutions for the coming years which we summarize below.
Cybersecurity as an ongoing priority
Looking further ahead and based on another report by IDC (used in the graphic and mentioned across this overview) that contains predictions regarding global healthcare IT and digital transformation evolutions at both payers and providers, we see how data is intensively used and transformational for the healthcare industry.
One obvious consequence is that cybersecurity is a key priority. That’s not just the case in the long run, to create a sustainable and secure digital healthcare ecosystem but also in the shorter term. IDC predicts that the number of ransomware attacks on healthcare organizations will double by 2018. We emphasized security earlier in this overview.
The move from passive to active patient engagement
According to IDC, 2017 is the year we move from passive to active patient engagement.
A factor that will contribute to patient engagement is the fact that we’ll see an increase of care plans that are adjusted in real-time thanks to the usage of AI/cognitive, in combination with wearables. IDC expects that as a consequence, 20% more patients will be actively engaged in their health by 2020.
The Internet of Things, Big Data and AI/cognitive
We can look at these three areas separately but obviously they are connected, with robotics as a fourth key component in the evolutions in healthcare transformation for years to come.
By 2019, IDC expects over 40 percent of organizations will use IoT-enabled biosensors. Moreover, as mentioned in the previous point expect an increase of wearables (in the context of care plans, monitoring and Big Data pattern detection although here we talk about other connected medical devices too). It’s been known since a while now that wearables will be important in healthcare. We’ve tackled the growing usage of wearables outside of the consumer context earlier and healthcare was already mentioned as one of the key drivers (healthcare & medical and fitness & wellness).
Healthcare and the Internet of Things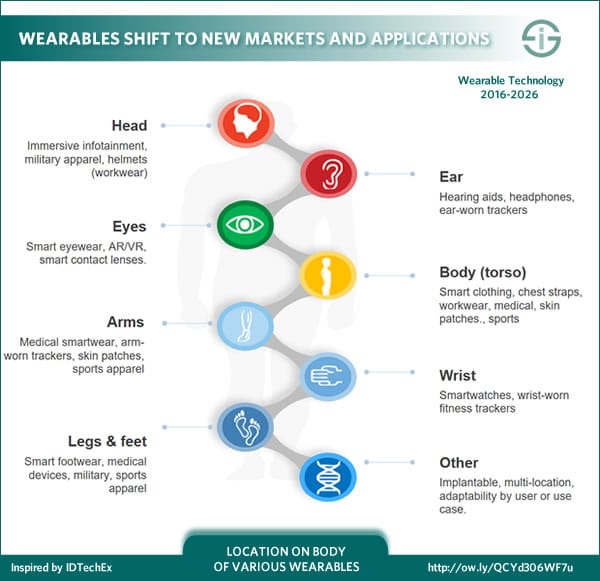
Freeing up time and resources: from real-time data to robots
Leveraging IoT, real-time location data and cognitive/AI, IDC expects that the detection of patterns will free up to 30 percent of clinician’s time.
That’s a lot. By 2019, 60 percent of applications in healthcare would already be able to do this. Other ‘automations’ which can save resources are the previously mentioned robots that can take care of time-consuming tasks.
Automation and data for the healthcare payers
On the healthcare payers side expect multiple ways of connecting premiums and so forth with healthcare data. And with RPA and process reengineering quite some costs will be saved.
Obviously there are far more ways to save costs, change payer models, free up resources and leverage new technologies. And we haven’t even fully touched upon the role of more recent technologies in health itself.
There is already a huge number of innovations, treatments and so forth based on advanced technologies and Big Data. And we haven’t even reached the first real evolutions in the fourth platform yet where the borders between human and thus also health on one hand and digital on the other further disappear.
Healthcare and digital transformation: EHR and data evolutions
As said, de facto quite some digital transformation projects revolve around information and data in order to enhance specific aspects of healthcare, solve challenges or come up with new healthcare models.
No wonder that information management plays an essential role here. In the overarching area of Health Information Management (HIM), electronic health records (EHR) have been an essential focal point in recent years. However, initially the attention for EHR didn’t correspond with the market reality.
In 2009, the Harvard School of Public Health found that just 1.5% of US hospitals had a “comprehensive EHR” in place and 7.6% a basic EHR. Nevertheless there was a consensus EHR could improve efficiency of healthcare service providers and there were differences depending on the size, location and scope of the hospitals (e.g. big hospitals).
The rapid evolutions in EHR adoption
Since 2009 quite some things changed in US healthcare but also in the adoption of digital technologies among businesses and consumers dramatically changed with digital transformation projects as a result.
Think about phenomena such as consumerization and the mobile revolution, for instance. The 2009 report also showed that resistance from physicians (36% of respondents) was an important cited barrier to EHR adoption in hospitals, although capital and cost issues were the main barriers.
Since then, things changed fast. According to a report by the Robert Wood Johnson Foundation, the number of US hospitals with a basic Electronic Healthcare Record system tripled from 2010 to 2012. As co-author Dr. Ashish Jha, an associate professor with the Harvard School of Public Health, was quoted: “Given the size of our country, that’s amazing progress in a very short time period”.
Still, there was (and in many countries is) a lot of work to be done, among others because although 42% of hospitals in the US now met federal standards for collecting electronic health data, only 5% met standards for exchanging that data with other providers. It’s exactly in this system of exchanging data that some other countries, such as the UK, were and are succeeding. It’s also a – much debated – topic where EHR evolutions are happening.
Among the reasons cited for the strong uptake in the previously mentioned uptake of EHR in the mentioned US research are:
- An increasing reliance on information technology, a phenomenon that marked the whole economy.
- New federal funding to support the purchase of EHR systems (just as in many other regions of the world).
- Future penalties under the Affordable Care Act.
The increasing adoption rate of EHR also showed the benefits, especially when the next steps were set (sharing of health data between providers): cost-saving by having a better patient view (e.g. avoiding duplicate tests), increased patient safety, etc.
Until 2020 the EHR/EMR market will continue to grow but at rather slow percentages and certainly less fast than many other connected healthcare segments.
Electronic healthcare records: putting patient and data care first
In an increasingly digital environment and society, at the same time concerns regarding security and privacy remained high.
Given the sensitive nature of patient records, government mandates, privacy concerns and security requirements, the healthcare industry has been relatively slow to adopt technologies with a higher perceived risk such as the cloud as well, for instance. But this is clearly changing as the healthcare industry amidst several innovation drivers (see below) is looking at how other industries use the cloud, among others from a data management perspective.
Data management, data governance and data quality are important challenges in the context of electronic health information records and healthcare information management. While data governance is about creating frameworks enabling IT and business work together in a credible and relevant way, data quality looks at the accuracy from the pure data perspective. Data governance involves rules for managing data in order to ensure data quality but also data integrity (whether the data is used in the correct context) and data usability (whether data and associated metadata are accessible).
The electronic medical record or EMR is a digital alternative for the good old paper chart while the more often used and broader electronical health record or EHR is the digital health “file” which is “attached” to the patient’s overall health history and is to be connected across the healthcare ecosystem whereas an EMR traditionally was more meant for an individual healthcare facility or clinician.
However, both overlap. Where data quality is an enabler (“the how”), data governance looks at the responsibility. However, both are about properly balancing and combining processes, people and technology with the goal of data and information optimization to meet business needs. Overall, innovation in healthcare IT is driven by a few important phenomena, many of them related with data. Data management, enabled by data governance (both are not the same), which at its turn is enabled by data quality, thus plays an increasing role.
Drivers in healthcare IT and transformation: efficiency and patient care lead in EHR
What do healthcare providers want from EHR systems? In a Computing Technology Industry Association Survey on Healthcare IT, there was an interesting overview of why healthcare providers adopt EHR systems from their perspective and what they wanted to see in EHR. In a special report on Healthcare IT, Computerworld made an interesting chart (full report here- PDF opens).
The top 4 reasons healthcare providers adopt EHR systems, according to the survey:
- Better patient care.
- Save time, improve efficiency.
- Reduce errors or the risks of errors.
- Improve staff productivity.
The improvements doctors wanted to see in EHR systems were a lot about speed, effiency and (thus ease of use) too.
The top 5 desired improvements by doctors:
- Increase speed.
- Easier to use, less complex.
- Lower cost.
- Removal of unnecessary functions.
- (tie): greater interoperability with other systems and better remote access.
The illustration below also shows the most commonly used EHR software features and the main reasons for not adopting EHR systems. These EHR adoption reasons and desired improvements indeed look a lot like several of the challenges we encounter as drivers for digital transformation in healthcare. Yet, how else could it be?

Digit(al)ization in healthcare: risks regarding the human dimension
As is the case in all ‘industries’, the increasing usage of EHR/EMR, the Internet of Things, digital technologies and data analytics in healthcare requires new skillsets.
In other words: healthcare facilities need to foresee budgets for training and/or new people who cannot just work with digital healthcare systems and remote health monitoring systems, as an example, but also can analyze and leverage the resulting data.
As healthcare organizations are already under pressure from a cost and staff perspective, there is a risk that this comes with a consequence for the existing workforce.
The balance between information-driven healthcare and human healthcare
If there is one area where the human dimension is crucial, however, it’s in healthcare. We cannot go to an over-digitized healthcare with a mismatch between the need for data and efficiency (costs) on one hand and the human touch of care on the other.
Health is a holistic given and every healthcare worker knows that diseases cannot be uncoupled from psychological aspects and human needs.
In the narratives around digital transformation and the adoption of the Internet of Things in healthcare we often hear about new business models, consumer engagement, costs savings, data analysis and so forth. Yet we rarely hear about this human dimension.
Consumer/patient engagement de facto often is used as a term to say that people have an obligation to take care of themselves, among others using those personal and other IoT solutions in the sphere of personal healthcare.
The underlying message as said is one of responsibility/accountability and reward/risk models: live healthy and get awarded, live unhealthy and don’t get awarded. While there is nothing wrong with personal responsibility and healthcare is under serious pressure, it’s essential to look at WHY people live in unhealthy ways, beyond the ‘data’ as human behavior is about far more than measurable aspects.
Root causes matter in the holistic reality of health
Just like human behavior is about more than 1,400 grams of protein and fat (the brain) as we mentioned in a context of customer experience and emotions, diseases are about more than symptoms, medication, data and so forth.
Many diseases are an outcome of a mix of root causes and require that the root causes are looked at too. As healthcare professionals know a big chunk of visits to doctors or healthcare facilities in the end has to do with emotional and psychological issues and just a talk or simple reassuring touch can do miracles.
In these times of efficiency, the root causes are often overlooked, as is the holistic dimension of health. Why does someone work out too less? Why does someone drink? Why does someone get ill, beyond the viruses and so on? Employment, relational issues, unconscious problems, it can all play a role. If we start organizing healthcare systems based on the personal behavior of people alone, which will increasingly happen in an age of remote healthcare monitoring, wearables and so forth, we risk to overlook the stressors and root causes of this personal behavior: unhealthy work circumstances, the never ending pressure to perform more and better etc.
The balance of digital and human skillsets: avoiding the shift of healthcare burdens in one area to another
Technologies can and do offer opportunities for patients to have interactions via video and so forth with healthcare workers. They enable people to improve health or connect with others to do so. However, if you take the example of remote health monitoring, this also means that you need to have those people who can listen and talk and understand the essence of care
In the current economy of efficiency, we can’t but notice that all too often efficiency and productivity of staff is mainly seen from a cost and essential care perspective and even in hospital settings patients do feel as if they are in a factory setting and lack essential psychological and human support.
This is obviously not a general phenomenon and all patients are different. It’s also not the ‘fault’ of healthcare workers.
However, if we don’t invest in people who are experts in the human dimension of care and focus too much on the digital and efficiency perspective and workers with those new skillsets we will trade efficiency in healthcare in one area for an increase of costs in another one: along with chronic diseases, mental issues are among the fastest growing ones and the latter take more than Big Data, IoT, fast remedies, technology, wearables, remote monitoring or pills to solve.
Next in healthcare: Paul Stoffels (Johnson & Johnson) on global health challenges
Top image: Shutterstock – Copyright: Sergey Nivens – All other images are the property of their respective mentioned owners.



