In our interview series on digital health and the digital transformation of healthcare we talked with mHealth (mobile health) expert Valerie Storms. Valerie has been closely involved in mHealth research & development projects and shares her views on how valuable mHealth applications are developed in collaborations between universities, hospital networks, government agencies, the industry and other stakeholders.
Since 2012, Valerie Storms is the program manager of the Mobile Health Unit (MHU), a center of expertise in mobile healthcare, so the lessons she shares are based on years of practical experience. The Mobile Health Unit is part of a collaboration between the university of Hasselt and hospitals in the region of Limburg in Belgium: Jessa hospital and hospital East-Limburg. Valerie has a master’s degree in ‘Bioscience Engineering: cellular and genetic engineering’ and a PhD in bioinformatics.
We will shift from a supply-driven to a demand-driven reality where patients will ask for a more convenient way of healthcare that takes place in their own environment (Valerie Storms)
The interview also touches upon several topics outside the strict scope of mHealth and the successes realized in this regard within MHU (including a spin-off with an FDA-approved application). Valerie among others also talks about the challenges to realize a multidisciplinary care approach, current care system challenges, health records and how to involve the patient better, starting from the education of doctors. An interview on mHealth with more than one personal twist since Valerie knows what it means to be a patient with chronic diseases, living with cystic fibrosis and diabetes.

Before kicking off: this interview series on the transformation of healthcare is conducted at the occasion of the 5th Conference on Digital Health, that took place early September 2019. Previous interviewees are Frank Dendas of Philips on, among others, the need for new healthcare models, Leonard Witkamp, on telemedicine and the current – according to him unsustainable – health system, and hospital network CEO Wouter De Ploey with the importance of hospital networks for digital transformation.
How a Mobile Health Unit creates an environment for education, research and innovation
Valerie, your presentation at the 5th Conference on Digital Health is entitled ‘Mobile Health technology, from bench to bedside’ so let’s talk about that journey in mHealth and start with the Mobile Health Unit: what is it and why was it launched?
Valerie Storms: The Mobile Health Unit is part of a broader collaboration between three partners in the province of Limburg in Belgium: Hasselt University, Jessa Hospital in the city of Hasselt and Hospital East-Limburg, which is in the city of Genk.
We want to stimulate a multidisciplinary approach, even for our medical students, whereby we also develop soft skills. We equally value empathy and communication with patients and that’s why we started a patient embassy at our university. Multidisciplinary and patient-centric care requires a shift in mindset, so we start doing it as early as possible.
In the province of Limburg, we don’t have an academic hospital and the cooperation between these three partners is a way to improve medical and clinical research in our region. Within that cooperation, MHU focuses on research and development in the domain of mobile health, in close collaboration with the industry and other stakeholders. We also support the development and validation of new digital sensor technologies enabling mHealth applications.
Was the fact that there is no academic hospital in the region a driver to start doing this?
Valerie Storms: Hasselt University and the regional hospitals already collaborated for the education of medical students since we have a faculty of medicine and life sciences where students can get a bachelor’s degree in medicine or a master’s degree in Biomedical Sciences.
This collaboration was a way to make it easier for our students to find internships without them having to need to travel too far. It enabled several win-win situations, also for the hospitals, for instance to attract talented doctors and staff with an interest in research and to create an overall research and innovation environment while helping the students during their education.
In 2012, this collaboration was formalized into the Limburg Clinical Research Center (LCRC) with a strong emphasis on clinical and medical research. Since 2012, more than 50 PhD projects were initiated.

The need for a multidisciplinary care approach: from soft skills to research challenges
Are first-line care providers and possibly other networks in the region involved too, keeping in mind the need for multidisciplinary care, one of the topics at the event?
Valerie Storms: Sure. We work together with the organizations of general practitioners and one of the questions that came up indeed was about the organization of a multidisciplinary care model.
MHU has research projects in many different disease areas like cardiovascular and respiratory diseases, renal disease, high risk pregnancies, orthopedics and solutions for patients with heart rhythm disorders
We really want to stimulate that multidisciplinary approach, even for our medical students, whereby we shifted towards having more focus on also developing soft skills: collaboration, communication and even empathy. For skills like collaboration our faculty works together with other faculties like ‘Rehabilitation Sciences’ or with the high schools where the nurses get trained.
But we also value empathy and communication with patients and that’s why we started a patient embassy at our university, which is a sort of ‘independent’ patient community of engaged patients that are involved in the education of medical doctors by sharing patient expertise and experiences.
We believe that multidisciplinary and patient-centric care requires a shift in mindset, so we start doing it as early as possible within the education of doctors.
Improving communication between different care providers with innovative digital and mobile health solutions
Valerie Storms: While in education that multidisciplinary approach is somewhat easier to put in place, in research it’s a big challenge that often requires a lot of resources.
It will be important to enable integration between solutions in various disease areas. Nor health care professionals, nor patients are willing to use separate digital tools, all with a different look and feel. Even more important, on the data level, integration is key to create much more opportunities and impact
Most of the time the resources for research are limited, also in smaller start-up companies and that’s why for the research projects we focus on smaller parts of the puzzle. So, answering the question what the Mobile Health Unit does: we try to connect primary physicians with specialists, with nurses, with physiotherapists etc. by digital solutions such as mobile apps and software that improves communication between these different care providers. However, when it comes to a multidisciplinary approach across different disease areas, that’s still a challenge.
We have research projects in many different disease areas like cardiovascular and respiratory diseases, renal disease, high risk pregnancies, orthopedics and solutions for patients with heart rhythm disorders.
I think, however, that it will be important to enable a kind of integration between these different solutions in the future. Nor health care professionals, nor patients are willing to use separate digital tools all with a different look and feel. But even more important, on the data level, integration is key to create much more opportunities and impact (precision medicine, predictive medicine, biomarkers,…).
Yet, that requires the involvement of larger companies with more resources and of the government to stimulate that these solutions which are now developed by smaller tech companies can easily interact with those of larger software providers such as providers of clinical record software for hospitals.
Today that is a challenge in getting a large-scale use of the applications that we develop with smaller companies and the research complex.
EMR and EHR applications standing in the way of mHealth innovation
So, multidisciplinarity is key in all aspects, yet harder to realize in the areas you mentioned and while you need to focus on specific diseases areas and mHealth applications, more means are needed with the participation of larger firms and government involvement. A question about the clinical record software you just mentioned. Being able to interact with it is key you say. For many interviewees these systems remain an issue. Most of the current ones come from an administrative background and interoperability seems to remain a problem. What’s your experience with them?
Valerie Storms: I can agree. At Jessa Hospital and Hospital East-Limburg the integration of hospital-wide electronic patient record systems is still ongoing too.
At Hospital East-Limburg a hospital wide EMR system from ChipSoft was implemented last year and there are still many challenges to structure the data in an optimal way to facilitate a broader use than only clinical follow-up. For example, using medical data for artificial intelligence and machine learning applications to really exploit the richness of the information in those electronic records.
There are many challenges to structure the data in EMR systems in an optimal way to facilitate a broader use than only clinical follow-up.
For Jessa Hospital it’s still an ongoing project: this year, they will make the transition to a new EMR system, KWS, developed by UZ Leuven. So, this means that you already have two local hospitals working with two different EMR software providers. You can imagine that for us, even if there are of course some groups of hospitals using the same system, that doesn’t make things easier.
Moreover, we often get feedback from industry players that for them it’s too expensive and time consuming to integrate their applications with the EMR of the hospital. Also, for the hospitals it is not always their priority. So, to evaluate the use of new digital care pathways, we work for the moment with standalone software next to the EMR system since we can’t always afford this investment. On the other hand, we still need to investigate the added value of these new digital supported care pathways, making an integration in an established clinical work flow not so straightforward.
Finally, the EMR software in hospitals often doesn’t enable to communicate with these standalone applications of new players as it often lacks the standardization to do so. The new, smaller industry players are ready but the hospitals don’t seem to be ready to work in this standardized way so there is a lot of work to be done I feel indeed.

Evolving from a supply-driven to a demand-driven healthcare system
Yet, sooner or later all these solutions will need to be integrated you said. Then you have someone like Leonard Witkamp who says that you’ll find a government will say they have chosen for the system as it is while insurers will say the traditional models already are so expensive, they can’t invest in these new technologies. Do you see the same issues regarding the mobile health applications in Belgium?
Valerie Storms: Yes, certainly. The government often looks at the short-term revenues when they invest, and of course, investing in new technology and prevention generates savings on the long term.
We need to convince governments to provide the right financial incentives and enable a framework where it is possible to exploit the benefits of new care models supported by digital technology, e.g. telemonitoring, telerehabilitation or digital diagnostics.
Evidence clearly shows that mhealth supported interventions can reduce hospitalizations or shift hospitalizations to the home situation…new approaches such as home hospitalization and telemonitoring enable to realize many savings in the future while meeting the changing demands of patients.
Since I believe we will shift from a supply-driven to a demand-driven reality where patients will ask for a more convenient way of healthcare that takes place in their own environment. I agree with Leonard Witkamp that we will shift towards a system that is closer to the patients’ environment instead of being too focused on hospital buildings. And all these new digital technologies like mobile health and telemonitoring are needed to support safe and accurate care outside the hospital.
For me, it’s just a matter of time before it happens, and I think that healthcare insurers and governments know that it’s the way forward but it’s an evolution and it takes time.
The evidence clearly shows that mhealth supported interventions can reduce hospitalizations or shift hospitalizations to the home situation and that these new approaches such as home hospitalization and telemonitoring enable to realize many savings in the future while meeting the changing demands of patients.
The value of mHealth – the patient’s perspective and need for new care models
One of the benefits of mHealth, telemedicine and so forth is that people in remote areas in theory can get easier access to care. In a small country like Belgium that challenge doesn’t exist, however. What do you see as the main benefits of mHealth and telehealth on top of some you’ve mentioned such as cost savings in countries like Belgium?
Valerie Storms: In our region the main advantage of technologies such as telemonitoring and mobile health is a more continuous view on the patient.
For people who have a chronic heart disease, or a respiratory disease or diabetes, to name a few, care is a daily challenge and it’s important to follow up these patients and get their parameters on a day-to-day basis so we can evaluate patient specific trends and deviations.
mHealth can make a huge contribution in areas where specialists or general practitioners are nearby in this sense. By getting accurate patient data, we can gather the information that can lead to early interception and faster intervention by using algorithms that pick up a worsening of diseases, enabling a simple intervention with medication instead of a hospitalization, with all the resulting benefits for the patient as well as for society.
Take the example of diabetes and the flash glucose measuring devices. You probably have seen that some patients have this kind of small sensor in their upper arm that continuously measures their glucose values. By flashing the smartphone over the sensor, the data becomes accessible on the patient’s smartphone and can be shared with the hospital. This technology has a huge positive impact for patients, making it easier to daily manage their diabetes. I speak from my own experience.
The shift will be from the current fee-based system to a quality-based system and value-based care models.
However, I think that the implementation and the use of this new source of information could be optimized. Health professionals only consult these remotely measured data when the patient is in the doctor’s office. In an ideal situation, a diabetes nurse or smart algorithm could triage between patients that really need specialist help, and patients that are doing fine and don’t need to go to the hospital. It’s not just about costs, it’s also about better care and the work of specialists. Patients with values that are way out of range, maybe should go more to the specialist than patients 90% in range. That makes the level of care more efficient and logical. Nothing so frustrating than traveling to the hospital and waiting for the specialist to hear everything is fine, while your diabetes management app could tell you exactly the same.
In other words: while mobile health offers great benefits it’s important to do it right, properly implement it and properly reimburse it or otherwise we will have new technology on top of an old way of organizing care.
That personal example certainly resonates, and similar ones come to mind. Yet, there’s the system, competition and money. Increasing revenues ranks high on the priority list of healthcare executives, ample stakeholders need to live, even if this often leads to unnecessary referrals and tests, the list goes on. Do you feel that the system is the biggest hurdle to change the system as Leonard Witkamp does?
Valerie Storms: I agree. As patients we’re often confronted with the fee-for-service system, which means a lot of examinations and consultations that could easily be avoided.
The shift will be from this current fee-based system to a quality-based system and value-based care models. Bundled payments will be important here: a system where healthcare professionals get bundled payments for a chronic disease, for instance, which they can spend to organize qualitative care in the best way possible, considering the efficiency and effectiveness of the way they organize it. And then they can also spend it on digital health technologies, whether it’s mHealth applications or others.
mHealth innovation in practice: the story of FibriCheck
Can you give an example of an application and how it was developed?
Valerie Storms: A nice project that you might know since it has received quite some media coverage is the FibriCheck application. It is the first Belgium-made medical smartphone application that was CE-certified and has FDA certification as well.
It started in the Mobile Health Unit, in 2013, out of a student project in Hospital East Limburg. The project revolved around the detection of heart rhythm disorders like atrial fibrillation (AF). AF doesn’t always have clear symptoms, so many people are not aware of it. But treatment of AF is key to prevent strokes. Detection is challenging as the abnormal heart rhythm may occur for a certain period and then turn back to a normal rhythm. That’s why patients often get a holter for a 24 hours ECG registration at home.
The question was if we couldn’t do something for these patients and we started a student project on the feasibility of a smartphone application to detect arhythmias. In the beginning it was more a technical project focusing on the PPG signal quality and developing algorithms. In 2014, this foundation was further developed into an application to automatically detect and assess the heart rhythm. That year, the research project was selected to participate to the ‘Health Ideator’ workshop of Microsoft Innovation Center, shortly followed by the nomination for Bayer’s Grants4Apps incubation program in Berlin for 100 days. That’s when my former colleague Lars Grieten, in the summer of 2014, took the initiative for the foundation of Qompium.
For medical use in patients, it was essential that the results of this PPG based smartphone application were as reliable and accurate as the current clinical (gold) standards and so the application was extensively validated in many different clinical trials and projects. In 2017, FibriCheck was one of the 24 mhealth pilot projects supported by the Belgian Government and RIZIV to investigate the clinical implementation and a reimbursement model for mhealth services.
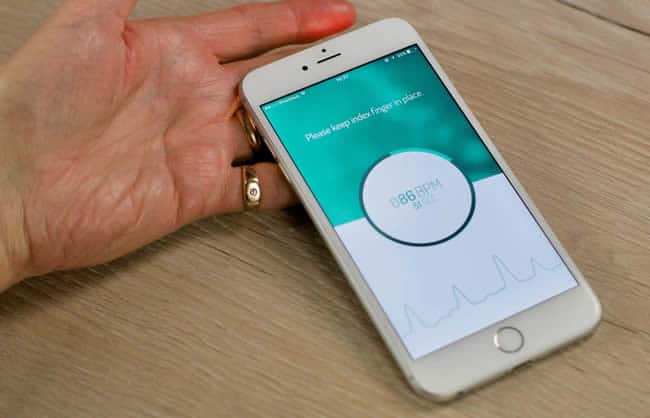
So, this is a nice example of how research is translated into a real and useful application, with already more than 125.000 users. Patients can download the app from the app store to use the software themselves and doctors can prescribe it, for instance to patients with a higher risk or to patients that had a medical intervention like an ablation or a kind of electroshock. It enables doctors to see if the rhythm disorder has really disappeared, if it comes back and if the treatment was effective.
Since a heart rhythm disorder can sometimes lead to a stroke the prevention aspect is important too and obviously with the app you can screen many patients and avoid the costs of in-hospital ECG examinations. So, the application offers quite some added value in many regards, it is low cost, convenient for the patient and highly accessible.
That’s indeed an mHealth application with real value. From a technology perspective, we’re in a connected environment using smartphone features whereby data gets uploaded to the cloud and artificial intelligence is used to analyze it?
Valerie Storms: Yes, indeed. The raw PPG signals from the patients are uploaded to the cloud where the algorithm is doing its work. They made the choice to do all analyses in the cloud since it allows to easier make optimizations and maybe even more important, analyzing the signals on the smartphone would require too much battery and processing power of your smartphone.
The classification of the signals is done in the cloud and the results are sent to the patient in the form of an easy to understand report with actionable data. In case the application was prescribed, the doctor can also follow-up the data of the patient in an online clinical dashboard, so it’s a closed loop between the prescribing doctor and the patient.
On the clinical dashboard, the doctor already gets an easy overview on all patients with color codes whereby green means a normal sinus rhythm, orange means doubt and a case to check and red means that the algorithm detected a rhythm disorder. Based upon these results the patient can then be referred to the hospital for an ECG and further controls.
Obviously, we conducted studies with many patients to investigate the diagnostic accuracy of the algorithms, those indicated a sensitivity of 96% and a specificity of 97% for AF detection. The algorithms get constantly fine-tuned and the more patient data are treated the better the algorithm will be as it’s continuously learning and optimizing based on patient data.
Supporting an ecosystem of innovative mHealth companies with research, tests and advice
FibriCheck is an example of an application born out of the collaboration you’ve set up in Limburg. Do you have a network that enables start-ups and innovative mHealth companies with an evidence-based approach and research to grow? A broader ecosystem?
Valerie Storms: Yes. We set up an ecosystem of hospitals and researchers whereby some companies are even located within hospital premises.
In Hospital East Limburg, for instance, we support the clinical validation process for Bloomlife, an mHealth company that develops sensor technology to monitor pregnant ladies, looking at parameters such as the heart rate and movements of the baby, and the contractions of the uterus of the mother. They have office space in the hospital and perform research on the topic of high-risk pregnancies and the prediction of preterm birth using their wearable sensor technology. We do something similar with Ectosense, a startup that is active in the detection and management of sleep disorders, more specifically the diagnosis of sleep apnea and of course there is ‘our own’ FibriCheck.
So, we try to bring companies really close to or nearby doctors, nurses, patients and researchers. We support them with the evidence-based way of working, the medical research protocols and getting ethical approval for conducting their studies on patients.
We also accomplished a structural collaboration with imec that funds PhD research in the hospitals to evaluate new clinical applications for their latest multi-sensor wearable technology. We try to nurture this network of start-ups and more established companies, working together with hospitals and academic researchers, and support them in getting the evidence they need, also for CE accreditation, enabling them to be recognized and further develop their activities.
MHU is further part of network organizations like Blue Health Innovation Center, Happy Aging, Flanders Health, In4Care and the VOKA Health community to partner up with all stakeholders.

The ingredients of a successful mHealth application according to Valerie Storms
This seems like a good time to talk about what makes mHealth applications successful or not. Here you clearly have the benefit of starting from a real problem and research leading to a solution, leveraging technologies such as IoT, cloud, analytics, AI and mobile.
Valerie Storms: It seems logical, but I think a successful mHealth application needs to be problem-driven. Sometimes we see companies that have solutions but that don’t really solve problems of patients, clinicians, hospitals or other stakeholders. Yet, there needs to be something behind the application that really makes a difference for one or more stakeholders, so they want to pay for it. Keep in mind that in Belgium patients are not used to pay for health care given the already high amount of taxes. And the government is focused on short term revenues.
There are many mHealth applications in areas such as fitness and wellbeing that also have their value, but you can’t really compare them with medical apps that have a proven medical and socio-economic benefit such as apps that support a personalized and comprehensive cardiac rehabilitation program at home.
A successful mHealth application needs to be problem-driven. There needs to be something behind the application that really makes a difference for one or more stakeholders, so they want to pay for it.
For example, Jessa hospital is a European leader in tele-rehabilitation strategies with many peer reviewed publications on the added medical value and the cost-effectiveness. Together with EDM (Expertise Centre for Digital Media) of Hasselt University, they partner in a seven-year H2020 project on personalized prevention for cardiac patients. This project is a fantastic opportunity to scale and implement a comprehensive tele-rehabilitation application which will be fully personalized, and which will evolve according to the preferences, the medical and the social context of the patient.
This is an example of a tool that has a clear proven benefit and improve the life of the patient in a personalized way which is less the case for many other applications that exist.
And then there is the user experience. Take an application for therapy adherence, for instance. I used one myself but each day you need to manually enter data about whether you took your medication or not and after two weeks you kind of get tired of that so, I think that it’s not just about clear added value for the user but that it also needs the least possible effort from patients so they will actually keep using it.
Valuable, personalized, evidence-based and the convenience that people want…
Valerie Storms: Yes, that’s one thing, it needs to be convenient. For example, sensor technology needs to have an unobtrusive form factor and a passive way of collecting patient information.
We did research on patients with pacemakers and implanted cardiac devices that really collect lots of data automatically, so the patient doesn’t have anything to do. That’s the ideal situation: effortless high-quality data in a continuous way.
Of course, that’s not always possible but striving towards the least possible patient action is key. As mentioned, we work closely together with imec that is specialized in several types of patches that collect reliable patient data without patients needing doing any effort and I think that effortlessness makes a huge difference. This sensor technology will be embedded in patches, clothes, bracelets, or even in your environment like your car seat or mirror.
You also need to communicate with the patient. All the relevant information that gets extracted from the raw data obviously needs to lead to actions and outcomes. Yet, you also need to provide actionable feedback to the patient on what the information means and what actions can be taken to improve their health, daily care or medical situation. Patients expect that.

Professional mHealth applications and the app store challenge
There are many mHealth applications. Some are less valuable than others, some are built by start-ups that haven’t really conducted any clinical research or didn’t publish any papers, yet they are all on the same app stores. Is it hard for companies with high-value medical apps to make the difference in that sense?
Valerie Storms: There are indeed many mHealth applications. As a university we need to work in a clearly evidence-based way and show that our app or service makes a clear difference through clear research.
We investigate if the difference is made in the clinical outcomes, in the quality of patients’ lives, in cost savings for specific stakeholders or for the healthcare budget….
So, the evidence behind an app is very important. People should also be informed about this because when you look in app stores you see many applications but there aren’t any rating systems, scores or marks that make it clear which apps are backed by evidence and research and which apps are more focused on living healthier and so forth.
A different type of app store or categories like a professional medicine mHealth app store?
Valerie Storms: Perhaps, yes. There are initiatives. In Belgium, for instance, there is an initiative from the Belgian government, Mobile Health Belgium, with a website where they have put all the CE grade medical applications which are backed by evidence and in the running for reimbursement.
That is a good initiative but I’m not sure if patients find their way to this website. So, I think that in the end also in the app stores there needs to be a mark that makes clear which apps are prescribed by doctors, used in hospitals etc. It would increase the confidence and ability to make an informed decision when patients decide whether to use a specific app or not.
Healthcare decisions for the future: time to be brave says Valerie Storms
Final question: imagine that you can have a talk with the Minister of Health in Belgium on what you think needs to happen in healthcare. What would you focus on?
Valerie Storms: I would definitely focus on the reimbursement of tele-monitoring services.
It is a good evolution that for type I diabetes flash glucose monitoring ‘technology’ is reimbursed. But that is not enough. The government needs to go a step further and create financial incentives for hospitals and medical professionals to shift towards remote follow-up of their patients leveraging digital technology.
Same story with implantable cardiac devices, the technology is reimbursed, but not the service to remotely check the disease and device parameters in order to support patients from a distance. This leads to the situation that patients need to come to the hospital for evaluation of their data, while they are remotely accessible. These unnecessary consultations could be avoided, costs saved, and patients satisfied.
So, politicians need to be brave and grab the opportunity to financially incentivize medical professionals to implement a digital service exploiting all possibilities of the digital technology. This will accelerate a patient-centered and demand-driven care model which is personalized, preventive and more efficient.
All pictures are property and courtesy of their respective mentioned owners.
Next in healthcare: Paul Stoffels (Johnson & Johnson) on global health challenges

