Telemedicine is key for the future of healthcare and already being deployed in many countries as part of digital health innovations. Ample start-ups offer telemedicine services and healthcare providers strike partnerships with some of them. An integrated approach around the patient is key to succeed but there are challenges. An interview with real-life lessons regarding telemedicine in the digital transformation of healthcare.

Prof. Dr. Leonard Witkamp is a former dermatologist and Professor in Telemedicine at the Department of Medical Informatics of the Academic Medical Centre in Amsterdam. He’s also the founder and director of KSYOS which he calls the first digital hospital in The Netherlands.
A fierce advocate of telemedicine, Leonard Witkamp is often interviewed on the topic and a regular speaker at healthcare industry events. On September 5th, Witkamp shared the lessons he learned and his views on the digital transformation of healthcare at the 5th Conference on Digital Health in Antwerp, Belgium.
Topic: the collaboration between first- and second-line care around the patient. Leonard Witkamp isn’t shy of controversial statements. One example: according to him by 2030 all hospitals in The Netherlands will be bankrupt for the reasons mentioned in this interview. Healthcare professionals will certainly also be interested in Witkamp’s views on the current leading electronic healthcare records systems (in a nutshell: expect disruption of the market).
Obviously, there’s a story and a vision behind the bold statements and strong opinions of Leonard Witkamp on future health developments and the challenges we encounter in care today. In this interview he shares some of these opinions, his vision, the experiences that led to them, the story of KSYOS and why the digital transformation of healthcare is nothing less than an urgent necessity.
80% of all cases in healthcare are low complexity routine cases
Leonard Witkamp, thank you for granting us some time. First things first: can you tell us about yourself and your background and why you started KSYOS?
Leonard Witkamp: As a dermatologist, I was really bothered by the fact that a major part of my work consisted of routine work and low complexity care which I could easily hand over to others. So, when I still worked in a hospital, I taught others to do these relatively simple care tasks which enabled me to focus on those patients needing specialist care: patients with complex issues, socially weak patients, acute patients and patients needing multidisciplinary care.
Yet there was still a high degree of low complexity care and I simply couldn’t handle it all. Gradually I started to feel like a production machine. That’s why I stopped being a practicing dermatologist and decided to realize my vision. I was convinced that if I could remotely supervise others, I would be able to do a major part of my job.
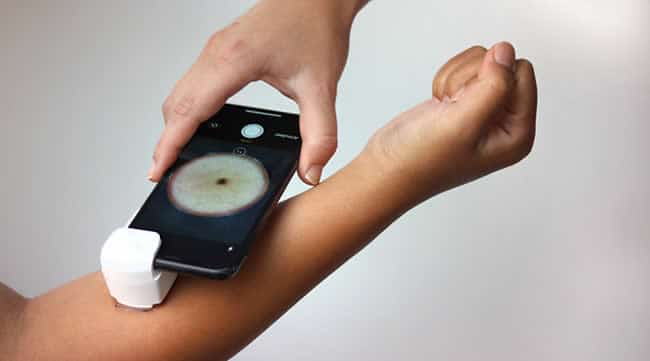
The Netherlands has a gatekeeper system with many general practitioners. By launching KSYOS I wanted to be able to remotely supervise those GPs – the gatekeepers – so they didn’t have to physically refer patients to me and the dermatologists I worked with. The GPs only had to provide some basic background on the patients and their conditions and send some pictures along. It turned out that in 80 percent of all cases patients didn’t need to come, simply based upon those pictures and the basic information.
It only took about two to three minutes for the dermatologists to look at each of those cases and there were no waiting lists. You can imagine what it meant that only 20 percent needed to be physically referred.
GPs also started asking for advice about patients they normally wouldn’t have referred physically. And sometimes we would find a lesion that raised the suspicion of a melanoma which of course we had to immediately refer to the hospital. So, it was better care in all senses: patients which didn’t need to see a specialist saved time as did specialists themselves, those that really needed to be referred didn’t have to wait and occasionally we detected potentially serious conditions. All stakeholders were happy, and it was a clear improvement of care quality, work satisfaction, patient satisfaction and the collaboration between first line and second line care around the patient.
Yet it didn’t stop with dermatology. Next, you expanded your activities to ophthalmology, mental health and more. How did that go?
Leonard Witkamp: Dermatology was indeed just the start. We expanded our activities to ophthalmology because the situation was even worse there. Many patients only came to the ophthalmologists for routine controls, for example retinal screening for patients with diabetes mellitus.
The waiting lists for these controls were very long. So, we started to monitor diabetic patients in retina pathology on diabetic retinopathy (DRP) and within three years we did this for about half of all the diabetic patients in the country. Here it’s the optometrist or the optician who has the proper machinery to take those screening pictures and the ophthalmologist, who would otherwise have to see these patients, does the remote supervision. Next, we took it a step further and extended this to other eye conditions such as glaucoma, cataract, macular degeneration. Today we work with over 200 ophthalmologists and 600 optometrists, taking care of the the major part of the routine, low complexity care.
A next step was mental health were again we saw that in secondary care all clinics were overcrowded but many people simply needed support and weren’t severely ill. So, here we started with a triage system to decide whether a patient could just get some support from family or rally needed to go through secondary care for more severe conditions or symptoms. The patients that didn’t really need this more specialized and dedicated help could stay in primary care with the GP who then was supported by either a psychiatrist nurse or a psychologist whom in turn were supported within a blended care system that enabled the patients to deal with specific issues to handle their diseases themselves with those paramedics. This has been successful too, with now over 4 million Dutch citizens having access to these programs.
Does this system also allow for some form of remote therapy with, for example, a psychologist, or online consults in acute cases?
Leonard Witkamp: No, we don’t focus on acute care. Everything we do is about these routine low complexity cases which in my view is around 80 percent of all cases in healthcare.
Combining convenience, better care and the end of long waiting lists
Today KSYOS is also active in pulmonology for patients with asthma or COPD, among others with spirograms, and in sleep research to detect sleeping issues with sleep apnea as the best-known example. Nowadays people indeed must go to a hospital for such sleep tests which isn’t the most fun or convenient thing to do whereas with the approach you have people can do it at home.
Leonard Witkamp: That’s one of the reasons why in my view this digital transition whereby we can deliver better care without any waiting lists closer to the patient is better in so many regards.
It’s far more convenient for the patient and it also comes at a fairer price. I used to say cheaper price but that’s not the main benefit and I prefer to focus at least as much on the others.
Sleep is indeed yet another example of this. Many people with sleep apnea or OSA (obstructive sleep apnea) don’t know they have it. For diagnosis they are referred to a hospital or sleep clinic where to have to stay at least one night.
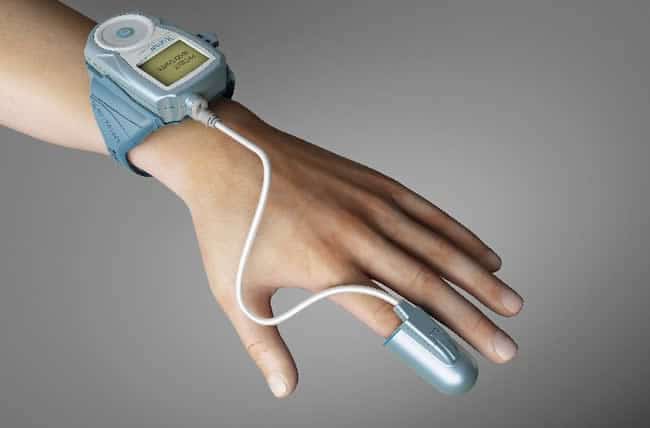
With our sleep recorder this can simply be done at home with some instruments placed on their body, typically on their hand. When one night isn’t enough as is often the case, they can get it for seven nights. Yet, the result is again a faster diagnosis, no waiting lists, convenience and the comfort of staying home, no hassle, less costs, the list goes on.
Bringing back the fun factor in healthcare work is key for Leonard Witkamp
Healthcare is a complex ecosystem with many intermediaries and stakeholders. Essentially you are transforming the ways low complexity care is done in all these areas. Moreover, you involve others more actively, for instance GPs and optometrists, and you reduce the interventions needed by specialists and hospitals. That requires a serious change of mentality and of existing practices. Is the mentality and the care system in The Netherlands different and ready for this?
Leonard Witkamp: The care system is an important factor. As mentioned, we have this gatekeeper system but there’s more. You can indeed imagine there are many thresholds in changing the way of working for everyone involved, health insurance companies, health workers, anyone.
However, the arguments are so convincing that even those who are reluctant in the end can’t deny the benefits and that’s what we clearly see in The Netherlands. I’ve always said that, in order to make our telemedicine approach successful it needed to be fun for everyone we involved in the chain and that’s what helped overcome reluctance.
Let me give you a few examples. In dermatology it’s fun for GPs to take the pictures themselves and not having to refer to the patient. And the reason why it is fun is because there is also a tremendous learning effect for the GP who gets the answer and advice in one day instead of having to wait for months for a letter from a hospital regarding a patient they referred when there are long waiting lists. So, there’s an instant learning effect.
Another example is ophthalmology. Patients get sent to the optometrist who really likes to be involved in this process, has a lot of knowledge but was neglected before. Medical specialists have fun because they don’t have to deal with routine tasks and low complexity tests or other activities for which they really weren’t schooled and they can play a remote supervising role, fully leveraging the expertise they do have. So, fun is a major part.
A second important factor is of course that they deliver better care. No one can deny that. And thirdly, well, healthcare professionals are afraid. The GPs are afraid they will get more work which isn’t paid, medical specialists are afraid they will lose patients but with our model they don’t have to.
However, it’s clear that the local situation and organization of care is a crucial factor in overcoming the hurdles to enable a similar telemedicine approach. While dermatology has been very successful in The Netherlands it would be much harder to implement in Belgium and the reason is simple: there are way more dermatologists per capita in Belgium so anyone goes directly to a dermatologist. So, it’s highly influenced by the way the system is set up.
However, the disruption is inevitable because the simple truth is that in the end the customer, the client, the citizen, the patient will become more and more powerful and choose digital care.
The main obstruction to transform the healthcare system is the system
The so-called digital and empowered consumers who want convenience and actively manage their own health are often cited as one of the main drivers of transformation indeed. What is the main force that slows down or even obstructs change in healthcare according to you?
Leonard Witkamp: The healthcare system is the most obstructing factor in the sense that the system wants to keep the system. The big promoter, on the other hand, is the individual. If I talk to you as an individual, you completely agree with me but once we start talking and thinking in terms of the system the resistance and doubt start.
You start getting objections and questions such as “OK, I see the benefits, but will my hospital go bankrupt?” or “What about my practice?”. Health insurance companies say, “We already pay so much with powerful hospitals and won’t pay extra money for these new initiatives unless hospitals effectively are less involved in care overall”. Politicians say, “Great but we decided that the health insurance companies are the one to get all this in place”. All these kinds of questions.
I compare the current situation a bit to that of the banks in 2008. They all were bankrupt but played such an important role that they were kept alive with the money of taxpayers. That was a good decision but now they are going bankrupt slowly.
And I think that the health system will also be kept as much and long as possible since it’s so important but it’s not sustainable. And that’s why I’m convinced that without any additional support, all hospitals will be bankrupt in 2030.
The hospital of the future: not the hospital you know
That’s a statement you indeed made before. On the other hand, there is a lot going on in healthcare facilities, including hospitals. In the US, for the second time in three years the top concern for hospital executives is improving ambulatory access, meaning adjusting facilities, staffing, hours of operation or throughput to increase patients’ ability to receive care across the health system’s outpatient locations, physician offices and clinics. In Belgium there is a plan to work more with hospital networks and revisit the organization of care with, let’s say, a more distributed and integrated model as we often see. And then there are hospitals where a high level of digitalization enables cost savings and better experiences across the board. What’s the future of the hospital for you?
Leonard Witkamp: I want to point out several things here. First, look at KSYOS. In the end we are a regular hospital with the differences being that we don’t have a building and complex automation, we don’t have a very expensive ICT system and we don’t have a layer of people working in our organization with the mere goal to maintain it.
In regular care 50 percent of all expenditure goes to buildings, IT, and people who aren’t working in the health process. Just from an economic point of view this simply isn’t sustainable. So, the way I see it those urban centers and hospitals doing everything will have to be downsized and focus on their core business: acute care, complicated care, multidisciplinary care and socially weak patients. Yet, these will not be hospitals but small and highly specialized centers with an ER and beds for truly ill patients. That’s one thing.
Secondly, on top of the fact that current hospitals aren’t sustainable it’s key to understand how people nowadays think and what they want. We want to organize everything from our couches: arranging holidays, watching movies, shopping, everything. And as a customer we like convenience. With a more digitally transformed model we can already be much closer to the patient than we are today and close the gap between what hospitals do and what people really want.
All this is completely possible. Today we need to call a hospital, it takes ten minutes before we get someone on the phone and then we get an appointment in six weeks. We don’t have to do all this.

I would even go further since until now I’ve been mainly talking about ambulatory, polyclinic and low complexity care but the changing behavior and demands from people will also impact what we want as patients who are hospitalized.
Ask hospitalized patients whether they prefer to be in a hospital that’s, let’s face it, today is anything but nice to be in, or a comfortable hotel with better care. A bed in a hospital room with four people easily costs 1,000 Euros per night. I personally certainly prefer a bed in a nice hotel at 200 Euros per night where I get the proper care.
So, on one hand there is this highly inefficient, very costly structure, and on the other there is a big gap between what the customer wants and what hospitals can deliver, a gap that keeps growing.
Are there any countries or regions that transform healthcare – or parts of it – in a way that you feel they can be a good example to follow?
Leonard Witkamp: It’s a little sad but in all honesty, I have to say I see very few good examples. In all countries the whole health system is struggling.
Now and then you see some things happening but, even then, they aren’t really examples to follow. Look at England, for instance. Slowly there is an opening to start doing video consultations with the main reason being the big shortage of general practitioners. Yet, on the other hand, video consultation now is highly inefficient because even then you have to organize for people to be there at the same time, etc.
So, no, I don’t really see good examples and the system again is the main challenge.
EHR/EMR software doesn’t do what it should: a market ready for disruption according to Leonard Witkamp
Let’s talk about another type of system than the healthcare system as such: the information systems that are, among others, used to consult and exchange information about patients, their treatments, their health etc. So, electronic or digital health and/or medical record systems. A survey by Philips recently showed that European healthcare professionals don’t use them that much and aren’t that satisfied about them than those in other regions, except for the US where it’s worse for various reasons that are well-known. What’s your perception of and experience with these systems? Are they important for the way you see the evolutions in healthcare that should happen? Have they become better than in the past?
Leonard Witkamp: I don’t think they have become better or improved things a lot. The information platforms in medical care are all administrative platforms.
Sure, they enable to handle patient files, the dossier, and they handle planning, logistics, billing and so forth but they don’t support the doctor or the patient in the health or sickness journey and the process of getting better because they come from these administrative systems. Moreover, they are ridiculously expensive so personally I don’t believe in these big systems such as Epic because they don’t get in the process itself. Moreover, they don’t enable to see any relation between the quality of a hospital and the way it’s been automated which isn’t even transformation.
Then what is a better option according to you? How do you work at KSYOS, for instance?
Leonard Witkamp: We have our own platform that is completely based on the patient journey. For any indication we build such a journey. Let’s take the example of ophthalmology. There is a complaint that is entered and based on the nature of the complaint the GP gets suggestions on what to do and what information to gather. Let’s say that the advice is that the patient should be referred to the optometrist. The optometrist then works in the same file on the same patient without any other systems involved. The ophthalmologist who supervises the whole process also works in the same platform, on the same medical data and within the same medical journey. That’s the only thing healthcare workers get to see.
Now, obviously the platform also generates administrative data which we use for billing, to make an appointment etc. However, for those things we use other, existing IT systems. Let’s face it: making an appointment is the same wherever and however you want to do it. So why build a system or buy an expensive one if there are very cheap alternatives and the focus needs to be on the medical process?
Sure, we make connections with other IT systems where possible to make life easier for the GP but in the end, we built up our own database with medical facts since we can’t rely on other platforms since they’re either not good enough or refuse to share data. And that’s what forced us to build that own databases, just as it’s the case anywhere in the world.
Too much focus on administration on billing. Too difficult and time-consuming. Not focused enough on the platform. Interoperability. The refusal to share data. That sounds indeed like quite some comments often hard about the types of big healthcare information systems you mentioned. Do you expect a disruption of the EHR and EMR market as we know it, given the evolutions you see and the mentioned shortcoming?
Leonard Witkamp: I certainly think so.
Connecting with the individual on all levels
That’s clear. There are ample start-ups and scale-ups in healthcare and obviously they need to have an ecosystem within which they can develop. What does it take to build a collaborative approach in a successful way?
Leonard Witkamp: First, it of course takes an entrepreneurial mind, a mission and a vision. The vision for us is that the current system is not sustainable and that the models for alternatives are out there with the many examples we’ve seen in the transformation of other industries such as banking, travel and so on with start-ups like Uber or Airbnb, for instance. Healthcare isn’t any different in this regard, it’s not rocket science. That’s the vision.
Our mission – and now we mainly focus on The Netherlands – is that in 10 years from now any Dutch citizen will work with KSYOS for their health. So, not for their sickness (alone), for their health. I really believe in public-private cooperation because we need the public institutions, but they need us as well since we all share the same mission. The new highly innovative entrepreneurs want to make healthcare better and that’s what everyone wants.
My recommendation is to reach out and go to the individual, not to the system since the system won’t help but the citizen will.
Globally there’s a trend whereby healthcare insurers aim to reward people who share health data and live healthier and, perhaps, even punish so to speak those who live less healthy. Now, health is a holistic given and people might have diabetes, smoke, drink and so on for reasons that are related to other issues. What are your thoughts on this?
Leonard Witkamp: In my view it’s never the role of health insurance companies to punish their clients when they are not living healthily.
Enabling people to live healthier, getting cigarettes out of the shops and so on is something for society and politics. What is good for health insurance is not to pay for sickness anymore but to pay for health, for outcomes. If you pay for sickness, you get sickness. If you pay for health, you get health. Simple as that.
And all focus and power to the patient and the clinician and their relationship?
Leonard Witkamp: Of course. And then I come back to my own motivation. Once clinicians are able to remotely supervise all this routine care which now makes them money but is not the best way to spend their time, their job satisfaction increases, and it becomes much more fun again since they can dedicate far more time with the patients they wanted to help in the first place, ever since they started their studies.
Then they can really spend a whole morning on one very complex case or talk to someone who has just been diagnosed with cancer for an hour, being empathic and looking at everything that can be done. That will make their job fun because, let’s face it, healthcare isn’t fun to work in anymore and it’s very difficult. We see that it’s harder and harder to get staff, for instance. At KSYOS we don’t have that issue.
A final question in the scope of that relationship between patient and clinician. You don’t like to talk about technology since it’s what it enables that matters. There is this perception that some technologies, and the EMR/EHR systems come back to mind here, have increased the time clinicians spend with their tablets, devices and systems, even in patient-facing circumstances. Is it a perception you encounter too?
Leonard Witkamp: Absolutely and it’s also why I’m very reluctant to talk about technology because technology is only a small part of what we’re doing.
In fact, the largest part of what we’re doing is all about change: changing people’s behavior, changing people’s perception, going to doctors and explaining them how our system helps them and their patients, conducting pilots, training clinicians, you name it.
That’s about 80 percent of our work and we don’t talk about technology with them but about design, how the system is designed, how it’s fun to work with and how, despite being technology, it can really offer them a completely different view, way to provide better care and platform to close the distance with patients, making their job so much more valuable and satisfying.
Thank you, Leonard Witkamp, for your time and views.
Next in healthcare: Paul Stoffels (Johnson & Johnson) on global health challenges

